Universal health coverage
Universal health coverage means that all people can benefit from quality health services, where and when they need them, without suffering financial hardship.

Universal health coverage has 3 key dimensions:
-
Access to health services: everyone who needs services should get them, not only those who can pay for them.
-
Financial risk protection: people should not fall into debt paying for treatment and care.
-
Quality of services: services should be adequate and effective.
Why is UHC important?
Many people around the world are not accessing the prevention services, treatment and care they need and to which they are entitled as a fundamental human right. UHC is about equity and fair access to health.
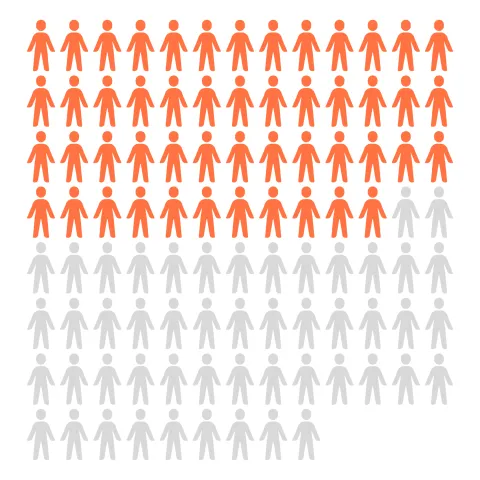
At least half of the world's population still lack full coverage with essential health services.
- At least half of the world’s population (7.3 billion people) still do not have access to the full range of essential health services.
- Over 800 million people (almost 12% of the world's population) use at least 10% of their household budgets for out-of-pocket health expenditures.
- Almost 180 million people spend a quarter or more of their household budgets on health.
- This population is increasing at a rate of almost 5% per year, with women among those worst affected (WHO/World Bank 2017).
- In a number of countries, the cost of cancer treatment and care, including cancer drugs, has pushed many cancer patients and their families to near bankruptcy.
- A study from India, for example, found that the odds of incurring catastrophic hospitalisation expenditures were nearly 160% higher for a patient with cancer than the odds of incurring catastrophic spending when hospitalisation was due to a communicable condition (WHO 2011).
COVID-19 has brought these issues of equity in healthcare and the right to health to the forefront of global conversations, and emphasised the importance of universal health coverage in building more resilient health systems and healthier populations.
*Sources: World Health Organization (WHO), World Bank, International Agency for Research on Cancer (IARC)
UHC and cancer control
Improving cancer control and providing access to life-saving services for all populations are steps towards Universal health coverage.
The first step towards ensuring equity in cancer care is recognising this and acting on it by improving access to care for marginalised communities in national cancer control plans that address the barriers to accessing care faced by underserved populations.
Investing in effective cancer care is certainly a cost – but this investment comes with a high return, as readily demonstrated by studies on scaling up interventions for childhood cancer, financing cervical cancer elimination and improving screening, treatment and quality of care globally.
UICC Podcast on Universal Health Coverage
The Social Determinants of Health
To achieve greater equity in healthcare, we also need to address the socioeconomic factors that contribute to disparities in accessing care and prevent many people from enjoying their full right to health.
Indeed, differences in income levels, employment, education and geographical location (rural or urban settings) as well as social norms and attitudes related to gender, sexual orientation, ethnicity, disability and old age also exert important influences on the way cancer and other diseases are understood, prevented, diagnosed, treated and lived by a person.
UHC can contribute to addressing many of these factors. UICC’s report “The Social Determinants of Health and Cancer” provides an in-depth look at how socioeconomic factors affect cancer care and how health inequity can be addressed through advocacy and action.
Political commitment to achieving universal health coverage
On 23rd September 2019, political leaders from around the world came together at the first United Nations (UN) High-level Meeting on universal health coverage (UHC) to mobilise political support and commit to achieving UHC.
The meeting saw the adoption of the 2019 Political Declaration “Universal health coverage: moving together to build a healthier world” which expresses countries’ support for UHC. This sets out a high-level framework for the development and implementation of national UHC plans with the engagement of civil society organisations and other stakeholders. The adoption is an important milestone for the global health community and offers several opportunities to strengthen cancer control.
UICC dedicated the 2019 edition of the World Cancer Leaders' Summit to the topic of Cancer and Universal Health Coverage. The summit ended with a strong call to action urging governments to fulfill their commitments and the entire cancer community to provide support and drive action.
A second high-level meeting on UHC will be held in September 2023. There will be several different opportunities for organisations and individuals to input into this process as UICC defines its advocacy priorities in the lead-up to the meeting.
Universal health coverage: background & political commitments
Replay of the webinar conducted by André M. Ilbawi, MD – World Health Organization (WHO).

Cancer advocates will need to take a proactive approach to champion the integration of essential...

Latest news and blog articles about UHC
Podcast "Let's Talk Cancer": Providing access to affordable, quality cancer care for all
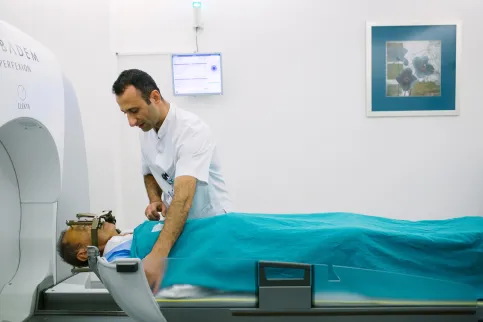
Essential cancer screening and diagnosis services must be included in UHC schemes to reduce mortality
Coordinating advocacy efforts is key to achieving UHC in cancer care
Last update
Wednesday 25 March 2026