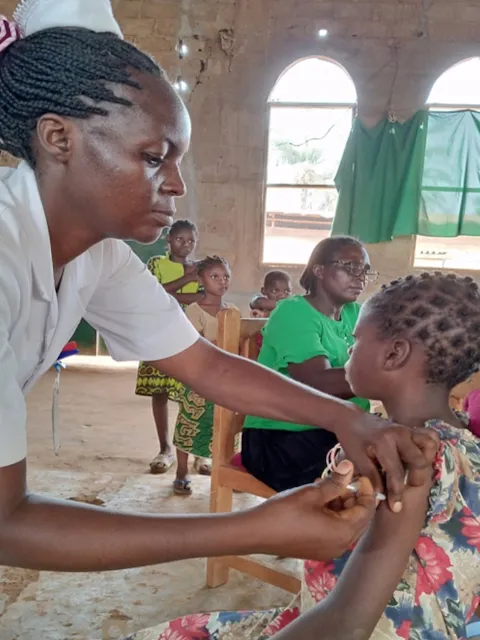
Improving access to HPV vaccine and screening in LMICs
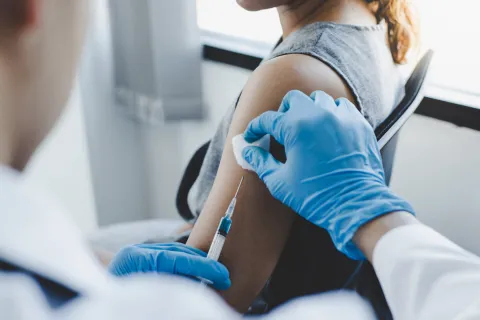
Marking International HPV Awareness Day on 4 March, UICC Young Leader Chemtai Mungo calls attention to current efforts to prevent and treat diseases caused by HPV, in particular cervical cancer, including improving access to HPV vaccines and new technologies for early detection.
Human papillomavirus (HPV) is a group of common sexually transmitted viruses. The virus is so common that up to 80% of people will be exposed to it at some point in their lifetime. Like many common viruses, most people will clear the infection with no consequences. However, infection with HPV can have significant implications for some, including HPV-related cancers.
Cervical cancer is the most common cancer caused by HPV infection. In 2020, an estimated 604,000 women were diagnosed with cervical cancer worldwide, and about 341,000 women died from the disease. Unfortunately, where a woman lives greatly determines whether she will be diagnosed or die from cervical cancer. Strikingly, 85% of cervical cancer cases are in low-and middle-income regions, such as South-East Asia, Latin America, and sub-Saharan Africa. As a result, 9 out of 10 cervical cancer deaths occur in low- and middle-income countries. This significant inequality results from the inability of health systems to offer proven prevention and treatment to women in these regions.
I was born and raised in rural Kenya. Like many people growing up in rural Africa in the 80s with limited access to health information and health care, I grew up believing anything "cancer-related" was a death sentence. This was because the few people I knew that were diagnosed with cancer died as a result. These were often painful and seemingly unpreventable deaths caused by late diagnoses or little to no access to treatment. I became an Obstetrician/Gynaecologist because I wanted to provide care to these women and reduce the unnecessary death and suffering I witnessed growing up in my community. I moved to the United States and ultimately fulfilled my dream of becoming a gynaecologist and clinical researcher.
During my medical training in the US, I quickly realized that the Kenyan and American prevalence of advanced cervical cancer is quite different. In particular, in America, I rarely encountered women with advanced cervical cancer; moreover, I have never seen a woman die from this disease. This is because women in the US have access to HPV vaccination and regular screening for cervical cancer. Vaccination against HPV prevents women from getting infected with HPV, the primary cause of cervical cancer. In addition, routine screening with an HPV test and/or pap smear facilitates early detection and treatment of cervical precancer before progression to cancer. The wide availability of HPV vaccination and screening in high-income countries has significantly contributed to the low mortality rate from HPV-related cancers.
In contrast, widespread availability of both early vaccination and screening in low- and middle-income countries is unfortunately rare. As a result, late-stage cervical cancer is a common diagnosis. In Kenya and Malawi, where my colleagues and I work, it is heartbreaking to observe that the gynaecology wards have many women who presented in the late stages of cervical cancer when the disease is no longer treatable. These late diagnoses result from a lack of access to screening and early treatment of precancer – the stage when the cancer is still curable. Consequently, women in these countries often die very painful yet preventable deaths. These dire outcomes are often coupled with social stigma and ostracism, which further exacerbates the impact of cancer in these communities.
Scientists and activists have worked hard to address this global inequality for decades. Following advocacy to enable the availability of the HPV vaccine in low-income countries at a subsidised cost and accumulation of scientific evidence of newer methods to screen for cervical cancer and offer precancer treatment even in rural areas with access to few doctors, we are at a critical period in history where we can address the unnecessary suffering and death from cervical cancer experienced by women globally.
In May 2018, the World Health Organization (WHO), led by the Director-General by Dr. Tedros Ghebreyesus, an Ethiopian Public Health researcher and the first African to lead the WHO, announced a global initiative to eliminate cervical cancer within the next century. This ambitious global strategy, adopted by the World Health Assembly in 2020, calls for all countries, including the most affected, to achieve the 90/70/90 targets by 2030. The global target calls for 90% of girls to be fully vaccinated against HPV by the age of 15, 70% of women to receive screening against cervical cancer, and 90% of women diagnosed with precancer or cancer to receive adequate treatment.
While these targets are highly ambitious, now more than ever, they are within reach thanks to recent innovations in science. Achieving them would mean a giant leap for womankind and equity globally.
Traditionally, screening for cervical cancer included a gynaecologic exam by a trained healthcare provider, a pap smear, and multiple visits before results and treatment. Recent evidence shows, however, that women can accurately self-collect their own specimens for HPV testing. This has significant implications, moving screening for this deadly but preventable disease from hard-to-reach clinics (in rural areas) to communities, markets, and even homes, which dramatically increases access to screening. Before treatment can be offered, a positive HPV test typically requires a working laboratory with a trained pathologist, often unavailable in rural settings.
Instead, current efforts are aimed at using artificial intelligence to enable highly accurate and immediate diagnosis from a cell phone image taken by a nurse or other health provider in a rural clinic, which can be followed with same-day treatment of women with precancer. In recent research from Kenya, we showed that incorporating smartphone images during screening was highly acceptable to women.
Eliminating cervical cancer is possible and, more than ever, highly probable in our generation, thanks to these exciting innovations. On International HPV Awareness Day, celebrated on 4 March, I join UICC in calling on all countries to be part of this remarkable moment, to urgently prioritise HPV vaccination of adolescent girls, and offer life-saving screening and treatment of women against cervical cancer.
Last update
Friday 18 March 2022Share this page