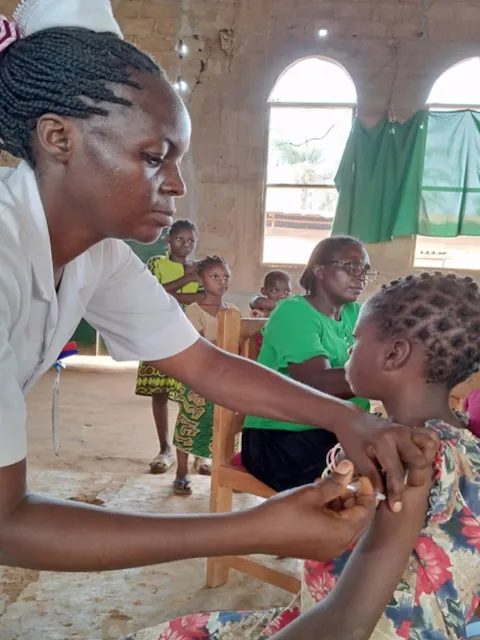
UICC engaged in supporting cervical cancer elimination in LMICs
While COVID-19 has slowed the progress of actions towards eliminating cervical cancer, UICC is committed to supporting its members and working with partners to realise the promise of the Global Strategy launched last year.

This 17 November marks the historic commitment made last year by the global health community to eliminate a cancer for the first time as a public health problem.
Key areas of action are outlined in the World Health Organization’s (WHO) Global Strategy to accelerate the elimination of cervical cancer as a public health problem and include:
- vaccinating 90% of girls aged 9 to 15 against the human papillomavirus (HPV);
- screening at least 70% of women aged 30 to 49 twice with a high-performance test and promptly treating precancerous lesions;
- and providing treatment to at least 90% of women identified with cervical cancer.
Globally, WHO estimates that achieving and sustaining these “90:70:90” targets will avert 74 million new cases of cervical cancer and 62 million deaths in 78 low- and middle-income countries in the coming decades.
Indeed, low-resource regions carry a massively disproportionate burden when it comes to cervical cancer and few diseases so starkly reflect global health inequity: 84-90% of all cases and more than 90% of all related deaths occur in low- and middle-income countries. Inequities exist even within countries; for instance, the five-year survival rate for cervical cancer in the US is 71% for white women, 58% for black women.
These discrepancies are generally due to lower rates of vaccination and screening, which lead to a later diagnosis.
The opportunity and promise of vaccination and screening
Cervical cancer is highly preventable through vaccination against HPV. A recent study conducted by The Lancet in the UK using real-world data showed that vaccination is cutting cases of cervical cancer by nearly 90%.
Here also, however, there is a significant gap between regions. HPV vaccination has been available since 2007, and over half of WHO Member States have introduced vaccination, but 95% of the 100+ million girls vaccinated between 2007-2017 lived in high-income countries where immunisation programmes are now routine.
Rwanda demonstrates that it is possible for low-income countries to achieve WHO targets. It was the first African nation to implement a vaccination programme in 2011 and 1.15 million girls had received a first dose of the vaccine by 2018 as part of this programme. Population-level coverage increased from 6% for girls born in 1993 up to a maximum of 99% for those born in 2002.
Rwanda also implemented in 2013 a Screen, Notify, See, and Treat cervical cancer screening programme for women aged 35-45 (30-50 for women living with HIV).
Indeed, cervical cancer is also highly curable when detected and treated early, but survival rates plummet when it is diagnosed at an advanced stage. For this reason, a routine screening programme, of which women aged 30 to 49 are aware and can easily access is critical.
Innovations in diagnosis and the use of artificial intelligence, as well as community outreach to remote populations and self-testing kits, hold further promise of achieving the elimination targets.
Overall, a comprehensive to implement HPV vaccination and screening in 50 LMICs could avert 5.2 million cases, 3.7 million deaths and 22 million Disability-Adjusted Life Years (DALYs) over ten years, at a total cost of USD 3.2 billion per year. According to WHO, "an estimated USD 3.20 will be returned to the economy for every dollar invested through 2050, owing to increases in women’s workforce participation, with this figure rising to USD 26.00 when societal benefits are incorporated."
Disruptions due to COVID-19
The COVID-19 pandemic, however, has disrupted many important health services. The COVID-19 and Cancer Global Modelling Consortium, of which UICC is a part, presented findings at UICC’s recent World Cancer Leaders’ Summit that highlighted the risk of a significant increase in cervical cancer-related deaths in 78 LMICs due to delays in vaccination, screening, treatment and scale-up of measures.
In many countries, a drop in vaccination rates and screening due to suspended routine programmes, or a reluctance to seek care out of fear of contracting COVID-19, will lead to worse outcomes for women with cervical cancer.
“The threat of a significant rise in cervical cancer-related deaths due to disruptions caused by COVID-19 to vaccination and screening programmes and treatment should serve to reaffirm global commitment to elimination and the importance of building more resilient and equitable health systems. An average of USD 0.40 per person per year in low-income settings is required to finance elimination through vaccination, screening and early treatment. Alongside the lives saved, the return is substantial in terms of improved health for women, higher participation of women in the workforce, and greater family and social cohesion and stability.”
– Dr Cary Adams, CEO of UICC
Supporting the cancer community to accelerate cervical cancer elimination
UICC continues to deploy a comprehensive set of activities in support of the implementation of the Global Strategy, for example, in working to increase access to screening and treatment in LMICs through SUCCESS (Scale-up Cervical Cancer Elimination with Secondary prevention Strategy), a project funded by Unitaid and led by Expertise France and delivered in collaboration with Jhpiego and UICC. The project supports four target countries (Burkina Faso, Côte d’Ivoire, Guatemala and the Philippines) and seeks to share the learning and expertise gained to other LMICs in the respective regions.
The project has overseen an expansion of HPV testing, training of clinical and laboratory staff, strengthening of diagnostic capacity and an increase in the number of devices available for the treatment of precancerous lesions. In addition, the SUCCESS project aims to mobilise and support civil society to raise awareness and advocate for improved cervical cancer screening and treatment, essential to long-term sustainability and the implementation of the Strategy at the national level.
In addition, bringing attention to the critical topic of health financing to achieve the elimination, UICC commissioned a report published in 2021 by The Economist Intelligence Unit entitled Global action on financing cervical cancer elimination: funding secondary prevention services in low resource settings. UICC is extending this work through national-level analysis of funding for cervical cancer control.
UICC is also working to sustain and mobilise political will at all levels. In May 2021, UICC helped establish the International Taskforce on Cervical Cancer Elimination in the Commonwealth, chaired by Dr Miriam Mutebi, a Breast Surgical Oncologist and Assistant Professor in the Department of Surgery at the Aga Khan University Hospital in Nairobi, Kenya and member of the UICC Board of Directors.
To help raise awareness about cervical cancer and support UICC members in engaging with the Global Strategy, UICC created a ‘cervical cancer hub’ that provides access to information, resources, videos, infographics, news articles and blogs about and from UICC’s members, as well as a series of Virtual Dialogues on elimination developed by UICC.
Specifically, for World Cancer Day 2021, UICC leveraged its global campaign to shine a spotlight on cervical cancer, and will do the same in 2022, helping its members to raise awareness of the disease and the opportunities for its prevention and treatment. Actions included the “30 Leaders initiative” where children asked global experts why and what they would do to address cervical cancer. A “21 Day Challenge” encouraged individuals to take small concrete steps towards understanding and raising awareness about cervical cancer.
Many of these initiatives, actions and collaborations will be pursued in 2022 to reduce the considerable gap in survival rates between low- and high-income regions and work towards ensuring that fewer and fewer women die from this preventable and curable disease.
Watch “Financing for cervical cancer elimination: Global, regional and national perspectives”, which highlights the key findings from the Economist Intelligence Unit’s report, moderated by Charles Goddard, Editorial Director at The Economist Group.
Watch “Modeling our way out of pandemic: Cancer prevention to treatment continuum”, organised by the Canadian Partnership Against Cancer. This session at UICC's World Cancer Leaders' Summit showcases the importance of data modelling in understanding the impact of the COVID-19 global pandemic on cancer, with an eye on pandemic recovery in the future.
Watch “Accelerating equitable access to innovative technologies for cervical cancer elimination”, organised by Jhpiego. This session at UICC's World Cancer Leaders' Summit presents examples of effective partnerships and approaches, recognising the role of all sectors in the implementation and scale-up of innovative technologies.
Last update
Monday 29 November 2021