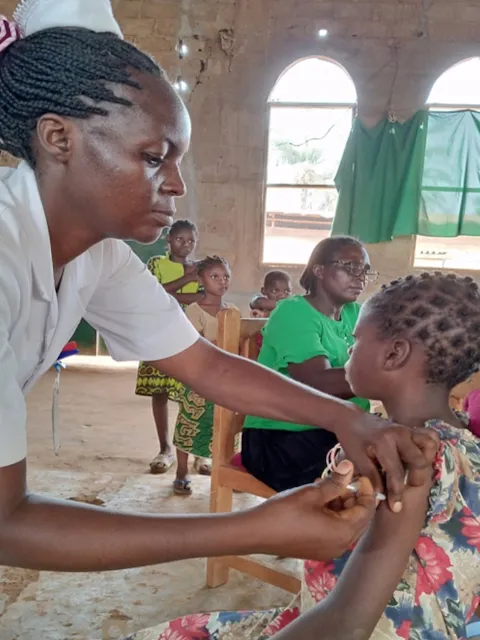
Improving data for decision-making: a toolkit for cervical cancer prevention and control programmes
This is a short interview by Julie Torode, Director of Special Projects, UICC with Leanne Riley – Coordinator of Noncommunicable Disease Surveillance at the World Health Organization and Mona Saraiya – Medical epidemiologist in the Division of Cancer Prevention and Control, Epidemiology and Applied Research Branch, Centers for Disease Control and Prevention. Thank you for joining us Leanne and Mona.

The UICC Treatment for All campaign calls on the international cancer community to address the global equity gap in access to cancer services by focusing on four essential pillars of cancer treatment and care.
A newly launched cervical cancer toolkit on data offers exciting data-focused technical assistance in line with this campaign, inspiring national action to save millions of lives by focusing on what needs to be done.
Julie: Thank you for choosing World Cancer Day to launch the Toolkit “Improving data for decision-making: a toolkit for cervical cancer prevention and control programmes”– who is the Toolkit aimed at and why?
Leanne: Following the call to action by WHO Director-General Dr Tedros in May of 2018, we are shaping a Global Strategy towards the elimination of cervical cancer. The emerging strategy, which is now entering a consultation phase, proposes a set of targets to be achieved by 2030 to drive the national comprehensive approach to cervical cancer prevention and control and put all countries on the pathway to elimination. In terms of screening we are proposing:
High coverage of screening for cervical cancer in women aged 30 to 49 years. Importantly, we are encouraging a shift to HPV testing as resources are available and ensuring all women with positive cases are followed to complete treatment of the pre-cancers or invasive cancers that are identified. Scaling up services will be a challenge for many low- and middle-income countries, this toolkit is well timed to support countries in their planning to save women’s lives.
Mona: Many countries do not have the capacity to harness data for program planning. The toolkit is carefully designed with the country in mind. It includes a standardised set of tools and resources to support the improvement of data systems and practices. As global efforts and initiatives related to cervical cancer continue to gain momentum, we hope this toolkit will help accelerate national action.
Julie: What components are included in the Toolkit?
Leanne: The Toolkit contains five sections, designed to be adapted to the country and programmatic context. Each section was developed to assist low- and middle-income countries in developing and strengthening their surveillance of cervical cancer screening and treatment.
Section 1: Rapid Situational Assessment of Data and Data Systems
Section 2: Population-based Survey Modules
Section 3: Patient and Programme Monitoring
Section 4: Facility-based Surveys
Section 5: Prevention and Control Costing: Analysis and Planning Module for Screening and Treatment
Julie: How did you test and validate the content?
Mona: An enormous amount of work ensured that the realities of on-the-ground implementation informed all of the tools and guiding information. Throughout the development process, numerous experts from international organisations, as well as national prevention and control programmes and implementing partners, participated in global consultations and contributed to toolkit content. Representatives from countries including Antigua and Barbuda, Botswana, Ethiopia, El Salvador, Georgia, Ghana, Guatemala, Honduras, Kenya, Madagascar, Malawi, Nigeria, Nicaragua, Senegal, Sierra Leone, Tanzania, Zambia and Zimbabwe generously provided input and review through various platforms. Four countries in Africa and one country in Central America collaborated with the project to conduct the Situational Assessment of Data and Data Systems (Section 1 of the toolkit) to inform country programming and to validate the tools and resources in the toolkit. Programmes in two countries in Africa collaborated with the project consortium to field test and refine the tools and content within sections 2 and 3 of the toolkit. The population-based survey modules in section 2 underwent rigorous cognitive testing; and the costing tool and process in section 5 went through a stringent review process, in addition to being field tested.
Julie: During past UICC/NCI USA workshops with country teams on this topic, we have found that many program leads did not have a good understanding of which facilities provided cervical cancer screening and treatment in their countries. In addition, costing and financial planning experience and expertise for the next phase of development of programs was considered a big barrier – do you have examples of countries that have used the Toolkit to address these gaps?
Mona: By working closely with country-based partners, we were able to develop a Toolkit that was practical for the user and responsive to existing needs. As you mentioned, one of the key needs is an understanding of which facilities provide services, and whether or not those facilities have everything they need to provide quality services. The tools and processes presented in Section 4: Facility-based Surveys directly address this need. The costing and planning tool in Section 5, as well as the materials in Section 4 related to minimum equipment and supply needs, were specifically designed to support country programmes with limited financial planning expertise.
As I mentioned before, there were several countries which participated in the field testing of various components of the toolkit. As part of this testing, one country used the facilitated costing tool and planning process to reassess the cost of their national cancer control plan. Those countries involved in the field testing of the tools and processes in Sections 3 and 4 continue to use them routinely.
Leanne: From the health financing perspective, we have been working with CHAI to support countries in developing costed national cervical cancer strategies. The Toolkit has been used in this work to ensure that all the necessary national data is collected. The scenarios tools are used to run through several implementation options and provide 5-year budget guidance.
Julie: The Toolkit is the result of a 5-year joint project between a consortium of partners – the CDC Foundation, the U.S. Centers for Disease Control and Prevention (CDC), the George W. Bush Institute (Bush Institute), and the World Health Organization (WHO) and made possible through a grant from the Bill & Melinda Gates Foundation to the CDC Foundation, how would you like to see the Toolkit used in the next 12 months?
Mona: I would like to see it used effectively by those countries which have a high burden of cervical cancer. They can explore their own data, use those data to develop or revise national strategic policies and plans, scale-up or introduce services, gain a deeper understanding of the existing burden, and the impact that the prevention and control programme is having on that burden. I would also like to see this toolkit serving as a well-timed supportive resource for the work that can be done under the Bush Institute, PEPFAR, and UNAIDS Partnership to End AIDS and Cervical Cancer. This partnership has put $30 million behind efforts to reduce cervical cancer deaths among HIV-positive women in sub-Saharan Africa and encourages the eight countries where it works to use data to drive.
Leanne: WHO aims to work with Member State to review the draft Global Strategy and Action Plan towards the elimination of cervical cancer in regional consultations over the next few months. Anticipating good progress, we would like to launch the Strategy for 2020 -2030 next year. I would like to see countries get a head start using the Toolkit to define the next phase of development of their screening and treatment programs and learn rapidly from the work reported from PEPFAR and UNAIDs collaborations for optimal progress towards cervical cancer elimination.
The Toolkit is currently available in English. Spanish and French texts will be published later this year.
Julie: The tag line for World Cancer Day is I am, I will, what’s your personal I am, I will commitment?
Leanne:
"I am Leanne Riley, WHO NCD Surveillance Coordinator, and I will support countries in using new WHO toolkit to collect high quality data on cervical cancer programmes. When high-quality data are collected and used to make decisions, prevention and control programmes are more effective and more women are protected."
Mona:
I am Mona Saraiya at the Centers for Disease Control and Prevention and I will support comprehensive surveillance and monitoring of cervical precancer and cancer using this WHO toolkit. What gets measured gets done.
Last update
Friday 07 June 2019