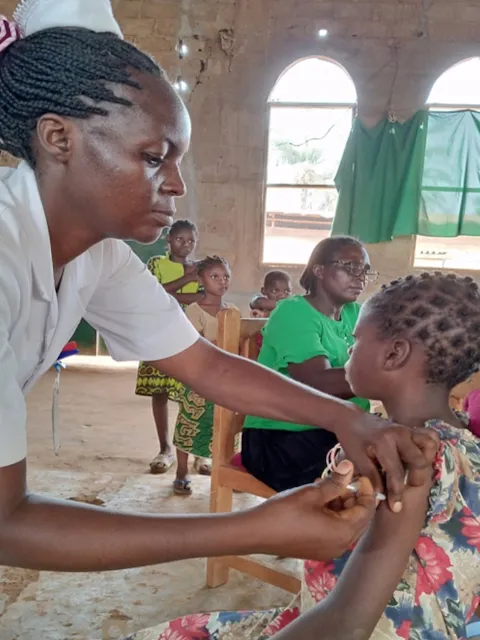
Cervical cancer elimination in Africa: where are we now and where do we need to be?
A new UICC report provides insights into the current situation of the cervical cancer burden in Africa, as well as recommendations to improve access to care and meet the cervical cancer elimination targets set by WHO.

Visit UICC's cervical cancer hub:
- What is cervical cancer?
- Causes, prevention, treatment
- How can it be eliminated?
- News and blogs
- UICC and member engagement
- Resources
Cervical cancer is one of the most highly preventable and, if diagnosed early, one of the most treatable forms of cancer. Some 70% of cervical cancers are caused by the human papillomavirus (HPV), a sexually transmitted infection for which there is an effective vaccine; and current screening modalities can detect pre-cancerous lesions at a stage when they can generally be treated successfully.
Yet, a woman dies every two minutes from cervical cancer and it remains the leading cause of death for women in 42 countries. A significant proportion of these deaths occur in Africa – all but one of the top 20 countries worldwide with the highest burden of cervical cancer in 2018 were in Africa – due to poor access to prevention, screening, early detection and treatment services.
Marking World Health Day on 7 April, UICC is releasing Cervical cancer elimination in Africa: where are we now and where to we need to be? This in-depth report, produced by UICC in collaboration with the International Agency for Research on Cancer (IARC) and the African Cancer Registry Network (AFCRN), looks at what steps are necessary in Africa to achieve the targets outlined by the World Health Organisation (WHO) in its Global Strategy for eliminating cervical cancer as a public health problem.
“Elimination” means that a country records fewer than four cases of cervical cancer for 100,000 people; in Sub-Saharan Africa, incidence rates are currently more than ten times higher. In moving towards elimination, WHO’s Global Strategy has outlined three targets for countries to achieve by 2030:
- Vaccination: 90% of girls fully vaccinated with the HPV vaccine by the age of 15.
- Screening: 70% of women screened using a high-performance test by the age of 35, and again by the age of 45.
- Treatment: 90% of women with pre-cancer treated and 90% of women with invasive cancer managed.
In addition to saving hundreds of thousands of lives every year, eliminating cervical cancer will also contribute to attaining certain Sustainable Development Goals. These include targets related not only to health but also to gender inequality, poverty and Universal Health Coverage.
To hope to achieve these targets, access to prevention, early detection, treatment and palliative care services needs to be increased. This will require support from heads of governments, local leaders, international agencies, civil society and relevant private sector organisations.
At the national level, African countries should prioritise cervical cancer control in national cancer control plans and align them with the targets of the WHO Global Strategy for the elimination of cervical cancer. Furthermore, people with cancer require financial protection so they do not face ruin from out-of-pocket payments.
The UICC report provides insights into the current situation of cervical cancer cases, deaths and services in Africa, as well as recommendations to improve access to care and reduce the burden that cervical cancer places on women, their families and communities.
These recommendations include covering cervical cancer services in basic healthcare packages; using existing testing platforms for other diseases, such as HIV and tuberculosis, as well as investments made in response to the COVID-19 pandemic (diagnostics, telehealth) to improve cervical cancer surveillance, screening and management; establishing reliable cancer registries; integrating prevention, detection and palliative care into other health programmes, particularly at the primary care level; exploring pooled procurement for diagnostics and treatment technologies; reducing stigma surrounding HPV and cervical cancer; implementing vaccination and screening programmes; improving access to oral morphine and essential supportive care services.
“Behind the numbers, there are real people. The 76,745 women who died from cervical cancer in 2020 across the African continent were someone’s mother, daughter, grandmother, aunt, sister, friend, work colleague, neighbour, caretaker… This is not inevitable. These women died from a preventable disease, which the global health community has the tools, the know-how and a path – and a moral imperative – to eliminate.”
– Dr Sonali Johnson, Head of Advocacy, UICC
Visit UICC's cervical cancer hub:
- What is cervical cancer?
- Causes, prevention, treatment
- How can it be eliminated?
- News and blogs
- UICC and member engagement
- Resources
Last update
Thursday 07 April 2022