Cameroon’s people-centred HPV vaccination campaign builds trust through mothers, churches, and community health workers
Florence Manjuh of UICC member CBCHS explains how misinformation, minimal staff training, and vaccine hesitancy in Cameroon have slowed HPV vaccination coverage. CBCHS is boosting uptake through healthcare worker training, church-based outreach, and integrated ‘mother–child’ screening and vaccination visits.
HIGHLIGHTS
- With national HPV vaccination coverage at only 36%, Cameroon Baptist Convention Health Services (CBCHS) has developed new approaches to overcome barriers to cervical cancer screening and HPV vaccination.
- A ‘mother–child’ approach and community advocates are strengthening trust and improving uptake among girls and boys aged 9–14.
- A UICC grant has enabled the expansion of church-based outreach in conflict-affected regions where children are not in school. Multilingual education materials and integrated clinic services are broadening awareness.
Florence Manjuh, a nurse and supervisor of the Women’s Health Programme at Cameroon Baptist Convention Health Services (CBCHS), a UICC member organisation, is outspoken about the loss of her elder brother to blood cancer. “It was so painful seeing him go through all he went through, I wanted to help others not experience the same,” she said, explaining how this loss shaped her decision to focus on cancer prevention professionally.
Ahead of International HPV Awareness Day on 4 March, dedicated to raising awareness about the prevention and vaccination of the human papillomavirus (HPV), Ms Manjuh spoke with UICC about the challenges Cameroon faces, notably in cervical cancer prevention and vaccine hesitancy, and how these are being addressed.
CBCHS launched one of the first cervical cancer screening programmes in Cameroon in 2007, the year Ms Manjuh started working at the organisation. In 2010, CBCHS was among the first in Cameroon to begin administering vaccines through a donation programme. “We were very excited to know that there were vaccines we could use to prevent this deadly disease, which had become a major burden in our communities,” she said.
The country officially introduced a national HPV vaccination programme in October 2020, just after the first wave of the COVID-19 pandemic. “Many believed the HPV vaccine was actually the COVID vaccine under a different name,” said Manjuh. “People didn’t want the COVID-19 vaccines, so they refused it.”
The rollout was also partly impeded by a lack of trained staff at many health facilities, according to Florence Manjuh. “The vaccine was available, but healthcare workers didn’t have the knowledge to administer it or explain it to the public,” she said. “We had to step in.”
CBCHS played a key role at the outset of the programme, and continues to support advocacy, awareness, and delivery, addressing misinformation and increase uptake. Indeed, coverage remains low, just 36% of the target population, according to 2024 data from WHO/UNICEF Estimates of National Immunization Coverage (WUENIC), far from the World Health Organization’s target of 90% by 2030.
Educating healthcare workers became a priority. CBCHS organised practical sessions to show staff real-life cases of pre-cancers and cervical cancer. “We showed them images of what we see in the clinics – cases before and after treatment,” said Ms. Manjuh. “That helped them understand the importance of prevention and how to talk about it confidently.”
CBCHS also identified persistent vaccine hesitancy as a notable barrier to the effective roll-out of the national HPV vaccine programme. “People also thought initially the vaccine was a form of family planning and would affect their daughters’ ability to have children later,” Ms Manjuh explained.
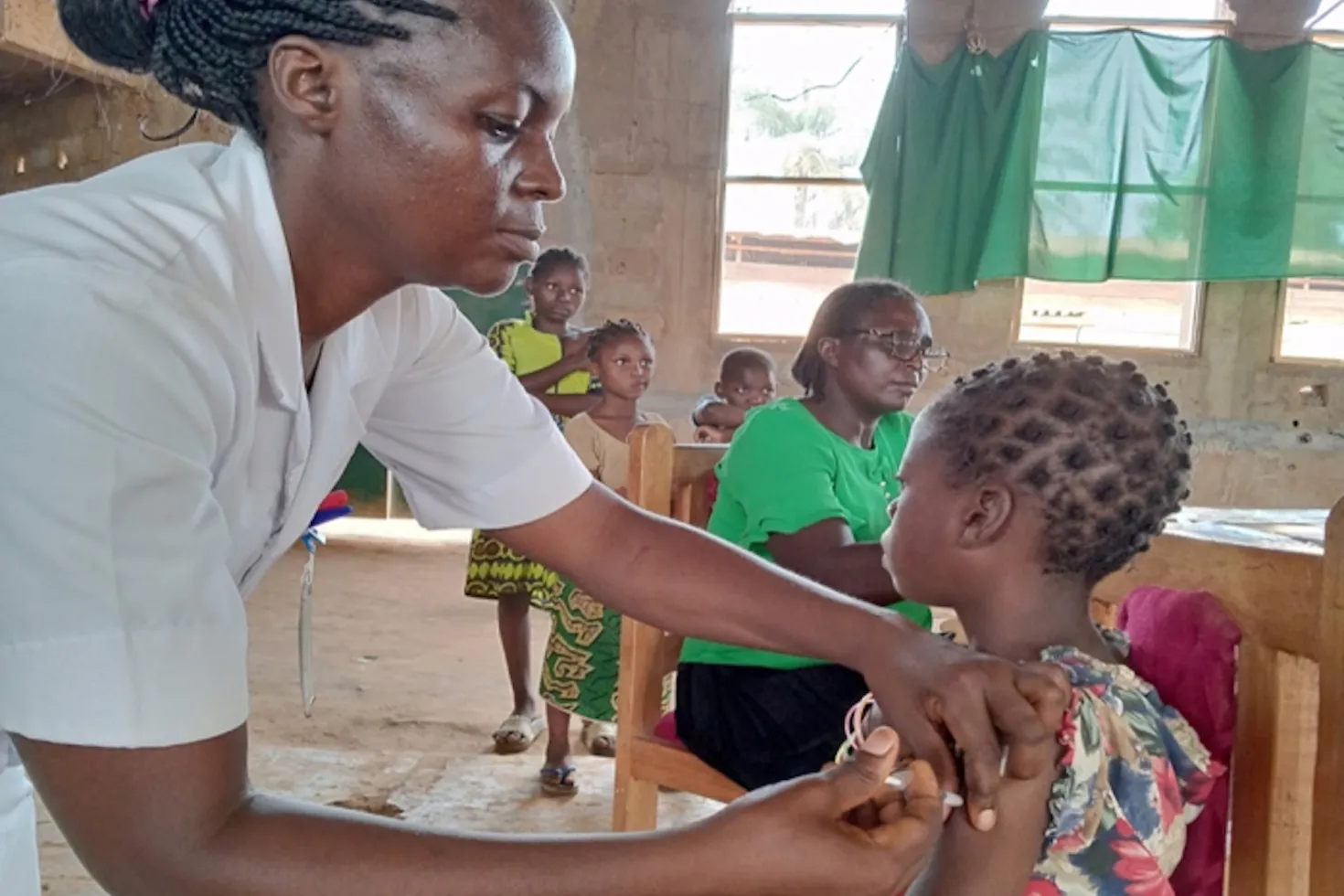
CBCHS developed targeted strategies built around trust and integration, notably with a ‘mother-child’ approach. Mothers are encouraged to bring their children for vaccination when they come for their own cervical or breast cancer screening, often after they have received education on HPV and its link to cervical cancer and other related cancers.
This approach was first launched as a 'mother-daughter' programme in 2022 with a grant from TogetHER for Health, training community members to sensitise families, screening women for HPV and vaccinating girls aged nine to 14. “Initially, it was easier with girls because mothers could relate directly,” said Ms Manjuh. A total of 613 women were screened and 1,892 girls vaccinated, about three girls vaccinated for every one woman screened.
The programme was then expanded to include boys as a comprehensive ‘mother-child’ programme. New concerns emerged, however, with some mothers questioning why boys should be vaccinated when they do not have a cervix. “But now we also explain that HPV can cause other cancers – anal, throat, vulvar, vaginal, and penile – also in boys, and that boys play a role in transmission. Once the risks to their children were better understood, mothers were more receptive, particularly if they’d been screened themselves.”
CBCHS also leverages its identity as a faith-based organisation. Churches across the country invite CBCHS to run awareness and vaccination sessions. “When information comes from the church, people are more likely to accept it, and churches trust us,” said Ms Manjuh.
Thanks to a grant received from UICC, CBCHS expanded this church-based model in the Northwest and Southwest regions. Because these areas are affected by conflict, children often do not attend school, and therefore cannot be reached by school-based awareness campaigns. The church-based model has therefore proven particularly effective in these areas.
Integrated approaches for women’s cancers
Integrated approaches for women’s cancers: Opportunities to advance health for women is a publication led by UICC that explores the current state of integrated approaches across women’s cancer care, from lived experience and service delivery to health system design. It highlights good practices, case studies and key gaps, drawing on contributions from the global cancer and health communities.
Outreach also happens through health facilities, where CBCHS integrates HPV education and vaccination into broader services. The organisation’s Women's Health Programme is a one-stop model of outreach clinics for women living remotely and in conflict areas, which offers family planning, screening for breast and cervical cancers, and treatment of reproductive tract infections. Posters in clinics advertise the availability of vaccines, and healthcare workers talk to patients about the full range of services.
“Even if someone comes only for family planning, we use that opportunity to tell them about cervical cancer screening and HPV vaccination for their children,” said Ms. Manjuh.
Women who have received treatment for pre-cancerous lesions are now engaged as advocates, sharing their personal stories to encourage others. “When they return for follow-up and see their pre-cancer is gone, they are happy,” Ms. Manjuh said. “They tell others about the value of screening and vaccination.”
Additionally, to reach Cameroon’s diverse population, CBCHS produces educational videos in multiple local languages, airs them on media platforms, and distributes printed materials such as flyers and posters. “Cameroon has over 250 languages,” said Ms. Manjuh. “We make sure the information is clear and accessible – in the language people understand.”
The combination of community outreach, integrated service delivery, and training of trusted health workers is helping CBCHS increase HPV vaccination uptake, though Ms. Manjuh notes there is still a long way to go. “We’ve made progress, but we’re not yet where we want to be,” she said. This work takes on added significance as HPV Awareness Day on 4 March approaches, highlighting global efforts to accelerate HPV vaccination and cervical cancer prevention.
Embedding sustainability: new approaches towards blended and sustainable financing for cervical cancer elimination
At UICC’s World Cancer Congress in Hong Kong in September, a session hosted by hosted by the Cancer Elimination Collaboration (CEC) and the University of Sydney will examine new approaches to blended and sustainable financing that can keep cervical cancer programmes going beyond donor funding, including how financing, workforce capacity and digital registries can strengthen long-term delivery and impact.
Discover the preliminary programme of WCC 2026 and register!
Last update
Wednesday 04 March 2026
