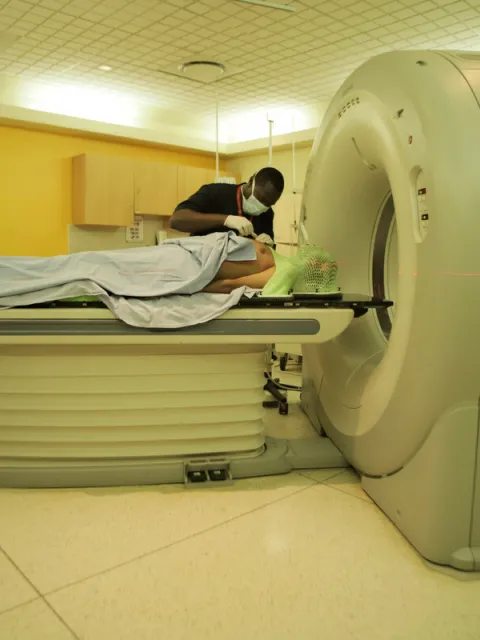
Community engagement and people-centred cancer care in India
Throughout July, UICC will be showcasing the work carried about by some of its more than 1,100 member organisations, starting with an interview with the Cancer Patients Aid Association (CPAA) in India, an organisation that addresses medical, social and economic barriers through community-based engagement.

HIGHLIGHTS
- Cancer Patients Aid Association (CPAA) has evolved from offering financial aid in 1969 to a holistic model that includes awareness, early detection, counselling, rehabilitation and advocacy.
- The organisation runs awareness and screening programmes in communities, schools, and workplaces to address stigma and promote early diagnosis.
- It provides integrated support such as treatment funding, food rations, transport and education assistance to reduce dropouts and improve outcomes.
- Vocational training in skills like tailoring and office work helps people who have experienced cancer regain independence and dignity, reflecting a whole-person approach to care.
Community-based approaches to cancer care are critical in closing gaps and improving access to services for underserved populations. Civil society organisations (CSOs) and patient advocacy groups play an essential role in addressing barriers such as stigma, financial hardship and delayed diagnosis, bringing services closer to those who need them most.
To understand what people-centred care means in practice, UICC spoke with its member organisation in India, the Cancer Patients Aid Association (CPAA), which has provided holistic support for people living with cancer for over five decades. Alka Bisen, CEO of CPAA explains how the organisation’s evolving approach addresses both medical and socio-economic needs and empowers communities across the country.
How has CPAA’s work evolved since its founding in 1969?
CPAA began by offering financial support to people who could not afford cancer treatment. But we soon realised that this was not enough. Cancer had become a much bigger problem than it needed to be due to a lack of awareness about the disease, myths, fear, and stigma, which was causing patients to present at late stages. People living with cancer face many interconnected challenges, so our model gradually expanded to include awareness generation, early detection, counselling, rehabilitation and advocacy. Our aim has always been holistic care – helping people from diagnosis through treatment and beyond.
How does CPAA carry out this mission, and help bring in more people-centred care into the health system?
We found that many people are afraid to talk about cancer. They may believe it’s contagious or always fatal. There is a fear that it may be passed on to future generations, thus creating problems in finding jobs or marriage prospects, always a worry in a society where even today a large proportion of weddings are arranged. So we run awareness programmes in schools, factories, housing colonies and women’s groups to correct these myths and encourage early medical consultation. We explain the signs and symptoms of common cancers – oral, breast, cervical and prostate – and urge people to seek help early.
What impact do these sessions have, and how do they lead into your screening programmes?
I remember a woman in a village who had a lump in her breast. Since it was painless, she ignored it, and didn’t tell anyone. After attending one of our sessions, she came forward for a screening. We diagnosed her early and she was treated in time. That is why awareness is so powerful – it can change lives.
Following our sessions, we also organise outreach clinics staffed by specialists – ENT surgeons (ears, nose, throat), gynaecologists, general physicians – who screen for the most common cancers. We go to places where people live or work, because many are reluctant to take the time to visit a clinic. Holding camps in familiar convenient settings with friends and neighbors makes it easier for them to come forward. Getting women to agree to get a pap smear done has always been a problem, so we work closely with NGOs already working with high-risk groups such as rag pickers and sex workers. We revisit the same areas regularly to follow up on suspicious symptoms detected until they are taken to a logical conclusion. Some people don’t follow up right away, but because we insist, they do eventually come once they’re convinced. There was a man who didn’t act on our advice for a biopsy initially, but did after repeated convincing. Fortunately, we caught his cancer in time.
What are the main barriers that prevent people from accessing cancer care, and how do you address them?
Fear and stigma are major issues. People are also held back by costs – treatment, travel, loss of income. Many wait until they’re very ill before they seek help. That’s why we focus not just on education and screening but also on financial and emotional support.
We help cover costs for chemotherapy, targeted therapies, and advanced tests like genetic profiling. We also provide food rations, help with school fees for children, and pay for transport. These services are vital. One young boy whose mother was in treatment stayed in school thanks to our support. Today, he’s studying to become a doctor.
How does CPAA influence broader access and prevention through advocacy?
We’ve challenged the evergreening of a patented drug, so that an affordable generic version could be made available in India, reducing the cost from over Rs 100,000 (approx. USD 1,150) to Rs 9,000 (just over USD 100). We also advocate for tobacco control – pushing for stricter laws and working directly with groups like auto-rickshaw drivers and police officers who are at high risk.
What does people-centred care mean to CPAA, and how is it reflected in your rehabilitation efforts?
It means looking at the whole person – not just the disease. We support people medically, financially, socially and emotionally. At our rehabilitation centre, we train people in skills such as tailoring, screen printing, box making, and office work, so they can earn an income and regain confidence. One woman who lost her job during treatment now runs her own boutique. That’s the kind of dignity we want to help restore.
Last update
Friday 04 July 2025