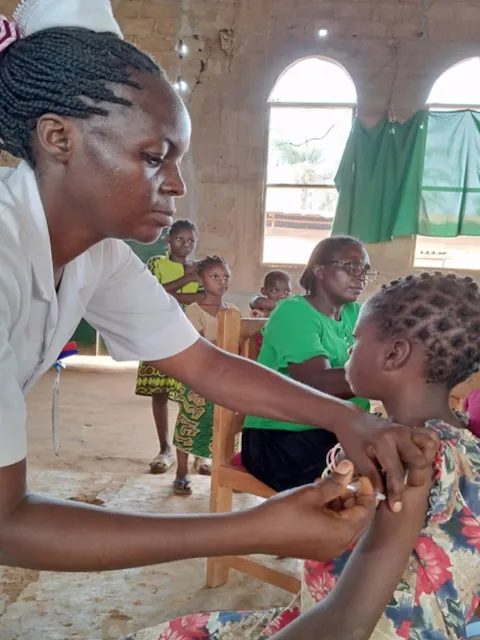
Cancer and HIV-AIDS organisations should work hand in hand to end stigma and fill service gaps

Women living with HIV are six times as likely to develop cervical cancer
In the human immunodeficiency virus (HIV) / Acquired Immune Deficiency Syndrome (AIDS) field, cervical cancer is known as an AIDS-defining malignancy. This is a type of cancer that a person infected with HIV is at high risk of developing. If a person with HIV develops one of these cancers, it means they have AIDS. Cervical cancer is an AIDS-defining illness since women living with HIV who become infected with HPV are more likely to develop pre-invasive lesions that can if left untreated, quickly progress to invasive cancer. In addition, HPV infection has been found to significantly increase the risk of HIV transmission for both men and women.
What many people are unaware of is that women living with HIV are six times as likely to develop cervical cancer and at a younger age – often hitting young women in their 20s rather than the usual 40s. Cervical cancer and HIV co-morbidity are high, women living with HIV can make up over 50% of cervical cancer cases in high prevalence countries. Thanks to HIV treatment, many more women living with HIV are living long and healthy lives, but to save a woman’s life by ensuring that she has access to antiretroviral therapy for HIV yet allowing her to die from preventable and treatable cervical cancer is unacceptable.
Girls and women at high risk of HIV and women living with HIV are therefore communities that must be a priority in national strategies to scale up cervical cancer elimination in line with the targets of the global strategy. Up-front investments are especially important to set high burden countries on the path towards elimination.
Like HIV, cervical cancer is a disease of gender and other inequalities between and within countries. These two interconnected diseases starkly expose the links between inequity and social and health injustice. Ninety per cent of 311,000 cervical cancer deaths globally per year occur in low- and middle-income countries, with the highest-burden borne by sub-Sahara African countries that have the highest number of HIV cases. Women are 10 times more likely to die of cervical cancer in eastern and southern Africa than they are in western Europe.
There is a growing awareness of the need to maximize synergies between the AIDS response and efforts to prevent, diagnose and treat cervical cancer. Existing HIV programmes are ready-made entry points for low-cost cervical cancer services and can play a strategic role in expanding cervical cancer prevention services to improve screening coverage for women. For this to be successful, we know civil society and communities have a central role. Networks of women living with HIV and women’s rights and youth movements are formidable allies for cancer prevention and control advocates. They have fought for an AIDS response rooted in human rights, social justice and sexual and reproductive health and rights and can mobilize, advocate and create demand for services, which is much needed if we are to eliminate cervical cancer. Cancer and HIV-AIDS civil society organisations working hand in hand will be key in holding governments to account on elimination and keeping us on track to end stigma and discrimination and fill service gaps as elimination services achieve the 90:70:90 targets.
Essential services that all women living with HIV have a right to access
Girls and women living with or at high risk of HIV should be a target population for all cervical cancer elimination strategies. Moving towards a people-centred health service means empowering this community to take part in maintaining a healthy cervix. Every girl and woman has a right to:
- Information on the interplay between HIV and HPV, the high risk of cervical cancer and the ability to prevent this cancer
- Information on signs and symptoms and the positive role of early detection and treatment
- Access to HPV vaccination at the appropriate age – a tool still missing the in HIV toolbox
- Access to high precision screening and treatment of any precancer from the point of HIV-diagnosis
- Access to early diagnosis, treatment and palliative care for invasive cervical cancer
- Robust monitoring for recurrence and survivorship care
Developing joint advocacy plans
UICCs growing membership is working to build national coalitions of civil society organisations that are partners to governments and take a focus on key cancer issues. I encourage cancer organisations and organisations working in the HIV-AIDS field to develop joint advocacy plans to raise the profile of cervical cancer in their communities and press their governments to take action to accelerate the elimination of cervical cancer.
If you want to connect with a cancer or HIV/AIDS organisation in your country, please get in touch and I will introduce you.
Want to get involved in World AIDS Day on the 01 December?
Check out these toolkits:
- https://www.hiv.gov/events/awareness-days/world-aids-day
- https://www.unaids.org/en/resources/documents/2019/world-aids-day-2019-communities-make-the-difference
The next opportunity to engage with the HIV-AIDS community
Last update
Thursday 21 May 2026Share this page