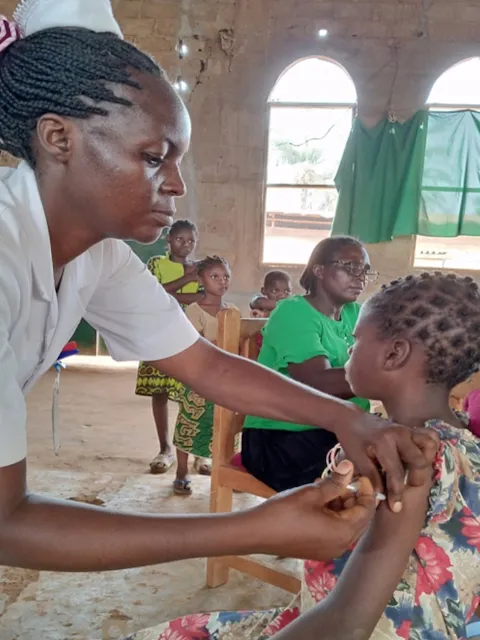
UICC members are closing the gap between services and the women who need them
Across the Philippines and parts of Africa, UICC members working to address women’s cancers describe a common set of barriers that keep prevention, early detection, treatment, and supportive care out of reach for many, notably due to high costs, remote living, and persistent stigma and misinformation.

Although cancer services may be available, many women do not access them or delay seeking care due to limited awareness of their existence or importance, particularly for prevention and early detection.
HIGHLIGHTS
-
Breast and cervical cancers remain the leading cause of death due to cancer for women in low-resource settings, in part due to stigma, low awareness, cost, and distance from services.
-
UICC member organisations such as the African Palliative Care Association and the Philippine Cancer Society are shifting care models towards community outreach, mobile clinics, and trusted local advocates to reach underserved women.
-
Mobile screening, structured patient navigation, and women-led peer education are proving effective in boosting early detection and linking women to timely diagnosis and treatment.
-
Persistent gaps – including high out of pocket costs, centralised services, and limited survivorship support – underscore the need for sustained investment and people centred cancer care.
Cancer organisations around the world are supporting efforts to address breast and cervical cancers, given these represent the leading causes of cancer deaths in many contexts, notably in low-resource settings.
Both can be treated effectively, less invasively, and at much lower costs for health systems and individuals, when detected early. In addition, cervical cancer can be prevented with vaccination against the human papillomavirus, and via screening.
Although services may be available, many women do not access them or delay seeking care due to limited awareness of their existence or importance, particularly for prevention and early detection. Even when women are aware of screening, treatment, and supportive care services, barriers such as cost, distance from service centres, and concerns about safety can prevent them from accessing care.
Eve Namisango is the Executive Director of the African Palliative Care Association (APCA), a UICC member organisation based in Uganda. The organisation works with governments, national associations, and service providers to support the delivery of palliative and comprehensive chronic care across several countries in Africa. This is done using various models which include, home/community-based, facility-based or tele-based, or a hybrid of facility and tele-based.
In her work, she often meets women whose cancers are already advanced. “This is due in part to stigma,” she says, “but also a lack of access to routine cervical cancer screening or early treatment services. Those involved in the informal caregiving role may not have the opportunity to go out for the screening services due to patient care demands or lack of awareness or availability of these services at primary care level. To bridge this gap, the services should be brought closer to the underserved, and strategies to achieve this include transportation to the clinic, outreach services, or home visits.”
In the Philippines, Dr Corazon A. Ngelangel, President and Vice-Chair of the Philippine Cancer Society (PCS), also a UICC member organisation, sees many of the same barriers. “Access is often shaped by where services are located,” she says. “Key services, including imaging, pathology, and colposcopy are centralised in Metro Manila and large cities.”
She adds: “In many areas, there is no consistent national screening programme,” meaning women are not routinely invited for screening and reminded to attend, such as regular mammography for women 50 and above. “Instead, screening may only happen through time-limited projects or when women seek it out themselves.”
Cost, low health awareness, and geographical location also delay diagnoses
This leaves women in geographically isolated and disadvantaged areas facing travel costs, lost income, and long waits for basic tests.
“High out-of-pocket costs for screening, diagnostics, and treatment deter women from seeking care, or lead to late presentation and treatment abandonment,” Dr Ngelangel explains. “Even with insurance coverage and national policies, costs can still reach hundreds of thousands to over a million pesos [just over USD 17,000] for some women.”
Ms Namisango describes lack of health awareness as a significant access barrier, particularly for women who live in remote locations, and girls unable to attend school. “School-based programmes do not reach them, so how are they going to know about cervical cancer – that it can be prevented, that you can even get vaccinated – unless somebody comes to see them at home?” she explains.
Both women also spoke about how discrimination and misinformation keep women and families from using services even when they are available. Dr Ngelangel notably identifies “fear, embarrassment, and stigma around breast and pelvic examinations,” alongside gender norms that push women to prioritise family and work over their own health. She describes modesty norms, stigma around reproductive health, and “fatalistic beliefs” as slow to change.
Ms Namisango speaks about the fears of screening and vaccination that circulate in communities in Africa, including beliefs that HPV vaccination could affect fertility. “Some guardians deny girls this service because they fear they may never have children,” she says. For her, this is not a communications problem alone, it is about who delivers information, where, and with what credibility.
Two models that bring care closer, and make it easier to accept
To address these barriers to access, PCS has built a service model designed specifically for communities that are least likely to access prevention and early detection. ACT NOW is a programme that uses a mobile, navigation-driven screening platform targeting underserved barangays (village or district) by offering on-site breast and cervical services. It also links women to diagnosis and treatment within a window of 30 to 60 days.”
“The model combines mobile, barangay-based events with structured patient navigation so women with abnormal findings are tracked, referred, and supported to reach diagnostic work-up and treatment initiation,” says Dr Ngelangel. Since 2022 April to 2026 February 7, ACT NOW has reportedly reached 381 barangays (1049 outreach missions), with 53,969 women who underwent a clinical breast exam, with 9% positive for a mass. These were navigated for further management to partner tertiary government hospitals; 33,180 women who underwent cervical cancer screening, with women receiving cryotherapy in the mobile clinic (one-stop), with subsequent follow-up visits.
“Early experience showed that single-day outreach without a defined pathway for follow-up care left many women without timely diagnosis or treatment,” Dr Ngelangel said. “This led to formalising the 30-Day Screening-to-Treatment model and strengthening navigation.”
In Africa, APCA, in partnership with the Rand corporation and the school of public health Makerere University, is bringing prevention and early detection closer to women’s lives by mobilising women who have previously been screened for or treated for precancerous lesions as reliable and convincing spokespeople.
“We have a six-week training programme that equips women with lived experience of cervical cancer to return to their communities as advocates,” says Ms Namisango. “These women in communities can reach bigger numbers than health workers can ever reach,” she adds, explaining that the programme trains women on how to start conversations and deal with resistance around cervical cancer.
When those women go back to their social networks, they ask others if they have ever been screened and share their own story. “We realised that when they do that, women do come to the facility and get screened,” she says.
The approach also allows for more integrated contact points. During a UICC-supported pilot project, ‘Increasing access to HPV vaccination and cancer awareness for girls and young women in informal caregiving for palliative care patients’, Ms Namisango says, women who brought their daughters for HPV vaccination were encouraged to undergo cervical screening as well as a breast examination. “Combining services in one visit can improve uptake, but it needs funding to scale and establish best practices.”
The case for women-led outreach is not only about increasing uptake. It is also about helping women complete their care when the barriers are social as well as medical.
“After treatment for pre-cancerous lesions, women may be advised to abstain from sex for six weeks. The doctor is not going to navigate that with you, so who is there for you?” Ms Namisango asks, describing how women may be financially dependent on a partner, may fear blame because cervical cancer is linked to a sexually transmitted infection, and may struggle to explain treatment and restrictions at home.
Dr Ngelangel also highlights survivorship gaps in the Philippines. “Structured survivorship programmes are rarely standardised, and access to psychosocial oncology, fertility preservation, sexual health counselling, and rehabilitation services remains limited, particularly in public and rural settings,” she explains.
As International Women’s Day is commemorated on 8 March, it is important to recognise these efforts and the progress these organisations are making in implementing effective people-centred cancer care for women in their respective regions.
At the same time, their stories highlight important gaps that remain in service access and delivery, and the need for sustained investment, policy commitment, and community engagement to ensure that every woman can access life-saving cancer care.
Last update
Friday 06 March 2026